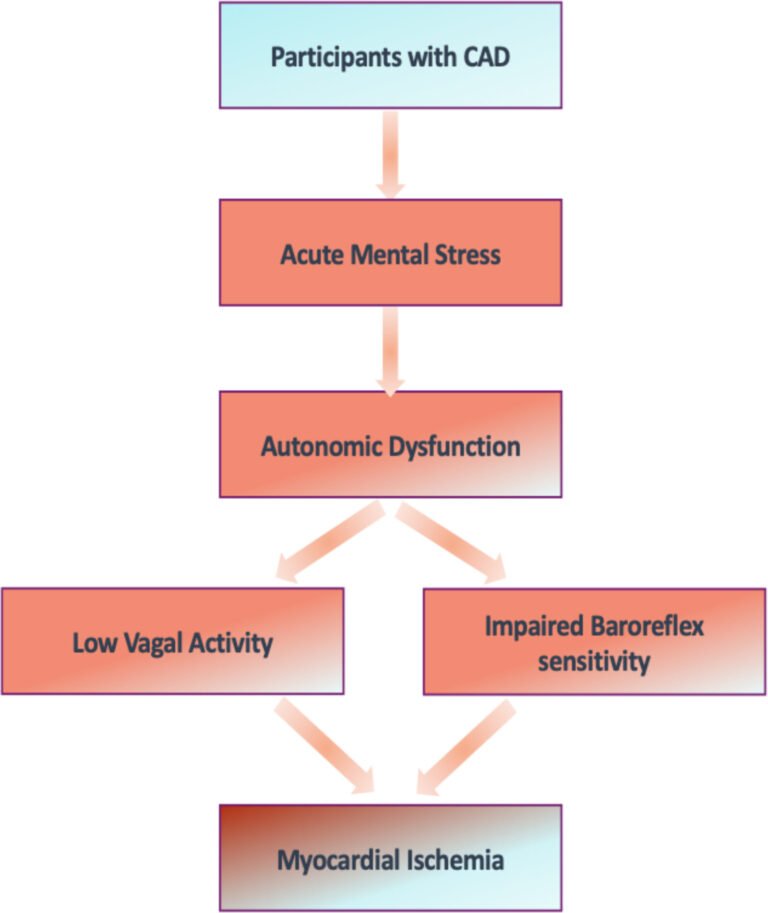
credit: Circulation: Cardiovascular Imaging (2024). DOI: 10.1161/CIRCIMAGING.124.016596
Imagine you’re walking through the park and suddenly you spot a bear. Normally, your heart beats faster and your blood vessels constrict. This is the sympathetic nervous system preparing your body for the “flight or fight” response. Then, when you reach safety, your parasympathetic nervous system calms you down. Eventually, your blood pressure and heart rate return to normal.
But some people with heart disease worry about the experience because stressful events can have further negative effects on the heart. In 2021, NIH-supported researchers found that one in six people with heart disease who experience mental stress are twice as likely to experience myocardial ischemia (reduced blood flow to the heart), which can lead to an increased risk of heart attack and heart-related death years later.
The same researchers identified a key mechanism involved in this phenomenon. Circulation: Cardiovascular ImagingThe researchers looked at the parasympathetic and sympathetic nervous systems, which help communicate between the brain and the heart, and found that a dysregulated response, as measured by reduced heart rate variability (the change in time between heart beats), may play a role in the increased risk of ischemia.
The discovery helps researchers understand what’s going on beneath the surface in patients with coronary artery disease who experience ischemia due to mental stress, said Rebecca Campo, PhD, program director of Clinical Applications and Prevention in the Division of Cardiovascular Sciences at the National Heart, Lung, and Blood Institute (NHLBI). “In general, a healthy response to stress is when your sympathetic and parasympathetic nervous systems are working in harmony,” she explained.
Campo noted that during psychological stress, the sympathetic nervous system kicks in and the parasympathetic nervous system recedes, like a seesaw. When the parasympathetic response is activated, this state is disrupted, and the physiological response to stress is tempered. Low heart rate variability may reflect dysfunction in these two systems and a dominance of the sympathetic nervous system.
The researchers wondered whether an imbalance between the two systems, also known as autonomic dysregulation, might be what causes ischemia due to mental stress. To assess this, the researchers measured heart rate variability to see if they could identify a connection.
It has been shown that high variability in heart rate reduces the ability to sense and respond quickly to stress. In other words, this shows that the autonomic nervous system is adaptive. If your heart rate is less variable, this could be a problem.
To test this in the lab, researchers evaluated cardiovascular outcomes in more than 700 adults who participated in the Myocardial Infarction and Psychological Stress Study 2 and the Mechanisms and Prognosis of Ischemia Induced by Psychological Stress Study 2 .
Participants were instructed to fast overnight and rest 30 minutes before the start of the exercise. They were then given a standard psychological stress-inducing task in the lab: preparing a speech about how they would react if they found out that a loved one was being abused in a nursing home. They were given two minutes to prepare their speech and three minutes to deliver it in front of an audience of at least three people.
Participants wore portable heart rate monitors to measure heart rate variability every five minutes before, during and after the task, and cardiac imaging was used to track heart activity and blood flow at rest and during the mental stress task.
The results supported the research team’s hypothesis: 119 participants, or 16 percent of the study sample, experienced myocardial ischemia during the mental stress test. Participants with the lowest heart rate variability, indicative of a poor cardiovascular response to stress, made up about a quarter of the study participants. The researchers found that these participants were twice as likely to experience ischemia during the mental stress challenge compared to participants with higher heart rate variability.
Amit J. Shah, M.D., a cardiologist at the Atlanta VA and an associate professor of epidemiology at the Emory University Rollins School of Public Health and lead author of the study, said there could be many reasons for the psychological stress response, one of which is a weakened heart that may have been caused by a severe heart attack.
That’s because the heart plays just as important a role as the brain in the functioning of the autonomic nervous system, Shah said. “They both have a say in what happens to your heart-rate variability,” he added.
Participants also underwent a traditional stress test, in which they walked on a treadmill until they reached their maximum heart rate. This type of physical stress did not elicit the same response as the speech exercises, supporting the idea that mental stress elicits a different physiological response in the body.
Shah and his colleagues, including first study author Geoffrey Osei, MD, MPH, noted that further research is needed to identify the specific pathways by which autonomic dysregulation leads to psychological stress-induced myocardial ischemia. However, findings from this and future studies may help advance research focused on ways to minimize these effects and support cardiovascular function.
For example, the researchers suggest that future studies could evaluate whether wearable heart rate monitors could help heart disease patients recognize early signs of stress and take steps to reduce their risk of heart disease. Other researchers might also study the effects of combining early detection with interventions such as aerobic exercise, yoga, deep-breathing exercises, or even medication for those at significant risk to help the body better sense and respond to stress.
“The more you can do to replenish and restore your body’s normal functions after a stressful event, including activating your parasympathetic nervous system, the more you’re helping your heart,” Campo said.
This research was supported by grants from the National Institutes of Health, including the NHLBI, the National Institute of Mental Health, the National Institute on Minority Health and Health Disparities, and the National Center for Advancing Translational Sciences.
For more information:
Geoffrey Osei et al. “Stress-induced autonomic dysfunction is associated with psychological stress-induced myocardial ischemia in patients with coronary artery disease” Circulation: Cardiovascular Imaging (2024). DOI: 10.1161/CIRCIMAGING.124.016596
Courtesy of NIH/National Heart, Lung, and Blood Institute
Quote: Mental stress linked to increased cardiac risk in heart disease patients (June 13, 2024) Retrieved June 20, 2024 from https://medicalxpress.com/news/2024-06-mental-stress-linked-heart-disease.html
This document is subject to copyright. It may not be reproduced without written permission, except for fair dealing for the purposes of personal study or research. The content is provided for informational purposes only.